Introduction
Epidemics and global health have always been closely intertwined. Throughout history, humanity has faced waves of infectious diseases that not only claimed millions of lives but also reshaped societies, economies, and healthcare systems. Epidemics are not just medical challenges; they are humanitarian, political, and social events that test the resilience of entire civilizations. From the devastation of the Black Death in medieval Europe to the rapid spread of COVID-19 in the twenty-first century, each outbreak has left behind critical lessons that influence how the world understands public health.
In today’s interconnected world, epidemics spread faster than ever before, crossing borders within hours due to international travel and trade. This means that global health is not just a matter of national concern but one of shared responsibility. Therefore, understanding the history of epidemics and global health responses helps policymakers, healthcare professionals, and ordinary citizens prepare for the future. Moreover, public awareness is vital, as epidemics are not merely stories of the past; they are ongoing threats that demand vigilance, preparedness, and cooperation.
Epidemics and global health challenges require coordinated responses, as highlighted by the World Health Organization’s guidance on epidemics. Experts at the Centers for Disease Control and Prevention emphasize the importance of early detection and rapid intervention. Global initiatives, such as those led by the United Nations on health, play a crucial role in ensuring equitable access to care. For real-time data on pandemics, the Johns Hopkins COVID-19 Dashboard provides comprehensive statistics and analysis.
The objective of this blog post is to explore epidemics and global health by reflecting on historical outbreaks, analyzing their consequences, and extracting lessons that can guide future action. In addition, we will look at how epidemics reshape healthcare systems, affect economies, and influence social behavior. Ultimately, the study of epidemics and global health demonstrates that every outbreak provides opportunities to strengthen resilience, improve medical innovation, and build more equitable health systems worldwide.
What Are Epidemics?
Epidemics refer to the sudden increase in the number of cases of a disease in a particular community or region, far beyond what is normally expected. Unlike pandemics, which spread globally, epidemics may remain localized but still cause devastating consequences. Epidemics and global health are interconnected because local outbreaks can quickly escalate into global threats if not addressed in time.
Historically, epidemics were often associated with poor sanitation, limited medical knowledge, and inadequate public health systems. In the modern era, however, epidemics can also be fueled by urbanization, climate change, and global travel. For example, diseases like cholera in the nineteenth century spread rapidly through unsanitary water supplies, while modern outbreaks like SARS and COVID-19 spread through international air travel.
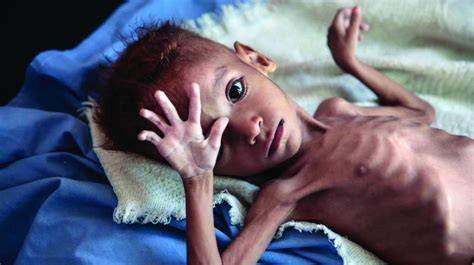
Moreover, epidemics reveal underlying inequalities in global health. Poor and marginalized communities are often the most vulnerable, lacking access to healthcare, clean water, and education. Consequently, epidemics expose the gaps in global health infrastructure and force societies to confront uncomfortable truths about inequality.
Another key distinction is between epidemic diseases that are new and those that re-emerge. Novel pathogens such as the H1N1 influenza in 2009 catch health systems off guard, while diseases like measles or tuberculosis reappear due to lapses in vaccination and public health vigilance. Therefore, epidemics and global health responses require constant adaptation, innovation, and coordination to ensure that both new and old threats are managed effectively.
Historical Outbreaks and Their Lessons
The Black Death (14th Century)
The Black Death, caused by the bubonic plague, swept across Europe between 1347 and 1351, killing an estimated 25 million people—nearly a third of the continent’s population. The epidemic revealed how fragile medieval societies were in the face of infectious diseases. Cities with poor sanitation and overcrowding became hotspots for transmission.
The key lesson from the Black Death is the importance of public health measures. Quarantines, though rudimentary at the time, proved effective in slowing the spread. Moreover, the pandemic highlighted the connection between social inequality and vulnerability, as poorer communities bore the heaviest burden.
The Spanish Flu (1918–1920)
The Spanish Flu remains one of the deadliest pandemics in history, infecting about one-third of the global population and killing over 50 million people. It struck during the final months of World War I, when soldiers and civilians were already weakened by malnutrition and stress.
A critical lesson from the Spanish Flu is that transparency in communication saves lives. Governments at the time downplayed the severity of the epidemic to maintain morale, which delayed effective responses. Therefore, open communication and timely dissemination of information are crucial in managing epidemics and global health emergencies.
HIV/AIDS (1980s–Present)
The HIV/AIDS epidemic reshaped global health policies. Initially stigmatized and ignored, it became clear that HIV/AIDS was not just a medical issue but also a social and political challenge. Marginalized groups bore the brunt of the epidemic, and discrimination prevented many from accessing treatment.
The lesson here is the necessity of destigmatizing diseases and ensuring inclusive healthcare. Global collaboration, activism, and scientific innovation eventually led to effective treatments, turning HIV/AIDS from a death sentence into a manageable chronic condition for many. This showed the power of advocacy and research in transforming global health.
Ebola (2014–2016)
The Ebola epidemic in West Africa exposed the weaknesses of fragile health systems. With a high fatality rate, Ebola spread fear across communities and overwhelmed local healthcare providers. However, global cooperation, including medical aid and education campaigns, eventually brought the outbreak under control.
The lesson from Ebola is the value of community engagement. Local trust in healthcare workers was essential to stopping the spread. Moreover, rapid mobilization of international aid demonstrated how epidemics and global health are inseparable in today’s world.
COVID-19 (2019–2022 and beyond)
The COVID-19 pandemic is the most recent example of how epidemics affect global health. With over six million deaths worldwide, it disrupted economies, closed schools, and reshaped everyday life. The pandemic highlighted both the strengths and weaknesses of global health systems.
Lessons from COVID-19 include the importance of investing in healthcare infrastructure, ensuring equitable vaccine distribution, and preparing for misinformation. Moreover, the pandemic emphasized how interconnected the world is: a virus that emerged in one city quickly became a global health crisis.
Global Health Systems and Responses
Epidemics have always tested the capacity of healthcare systems. A robust global health infrastructure is vital to contain outbreaks before they spiral out of control. Epidemics and global health responses depend on several factors: early detection, efficient communication, medical preparedness, and community trust.
The role of organizations such as the World Health Organization (WHO) has been pivotal. WHO coordinates international responses, provides technical guidance, and ensures that resources reach vulnerable populations. However, epidemics like COVID-19 revealed gaps in coordination, resource allocation, and political cooperation.
National health systems also play a crucial role. Countries with well-funded, inclusive healthcare fared better during epidemics, while those with weak infrastructure faced overwhelming challenges. For example, South Korea’s early testing and tracing during COVID-19 became a global model, whereas countries with delayed responses saw devastating consequences.
Moreover, epidemics highlight the importance of research and innovation. Vaccines, antiviral drugs, and diagnostic tools are products of scientific progress that can transform epidemics into manageable health issues. Therefore, global investment in medical research must remain a top priority.
Consequences of Epidemics on Society
Epidemics and global health crises extend beyond medical concerns. They reshape societies in profound ways.
Economic Impact
Epidemics disrupt economies by reducing productivity, shutting down industries, and straining public resources. COVID-19 alone caused the worst global recession since World War II. Historical epidemics like the Black Death also reshaped labor markets, leading to significant social change.
Psychological Effects
Epidemics generate fear, anxiety, and stigma. Communities often respond with panic, discrimination, or scapegoating. For example, during the early days of HIV/AIDS, misinformation fueled discrimination against certain groups.
Social Inequality
Epidemics magnify inequality. Marginalized populations are more likely to be affected due to limited access to healthcare and education. This creates cycles of vulnerability that persist long after the epidemic ends.
Political Consequences
Governments are often judged by how they respond to epidemics. Transparent, decisive leadership builds trust, while denial or incompetence leads to public backlash. Epidemics, therefore, influence political stability and governance.
Preventing Future Outbreaks: Lessons Learned
The study of epidemics and global health provides essential lessons for the future.
- Strengthening Healthcare Systems – Universal healthcare and well-funded infrastructure are non-negotiable in epidemic preparedness.
- Investing in Research – Continued innovation in vaccines, diagnostics, and treatments ensures faster responses.
- Improving Communication – Transparent, timely information builds trust and prevents panic.
- Ensuring Equity – Global health must prioritize vulnerable populations to prevent inequality from worsening.
- Global Cooperation – No country can fight epidemics alone. International solidarity is essential for effective containment.
Conclusion and Call to Action
Epidemics and global health are inseparable themes that define humanity’s past, present, and future. Each outbreak carries devastating consequences but also valuable lessons. From the Black Death to COVID-19, epidemics remind us of our shared vulnerability and interdependence. Therefore, preparing for future outbreaks requires investment in healthcare, commitment to equity, and global cooperation.
Ultimately, epidemics teach us that resilience lies not in isolation but in solidarity. The lessons of the past must guide the present so that the future of global health is stronger, more inclusive, and better prepared for the challenges ahead.